You can’t help but wonder about the tell-tale signs that might mean extraction is in your future. It’s common to have some pain that comes and goes, a tooth that looks just fine in the mirror, and this nagging little voice in the back of your head telling you something’s just not right with your oral health.
Having a tooth extraction is common enough, but it’s generally not the first line of defense. Your dentist will try to save that tooth and only recommend removal when keeping it is more of a gamble than a guarantee.
Dental Issues that might indicate that you need a Dental Extraction
A tooth can look fine in the mirror, but could be failing under the surface, big time. Extraction is usually the way to go when there just isn’t enough healthy structure left to support a reliable restoration.
- If you are experiencing severe tooth pain that just won’t quit
- Swelling, a bump in the gum tissue, or some nasty drainage (pus)
- A tooth that feels loose, no matter how old you are
- Broken teeth with cracks that look like they go way below the gum line
- Severe tooth decay with pretty much nothing left to work with
- Failing repairs on the same tooth: it’s happened before, but keep in mind those repairs might not be the same as new ones
If you’re told a tooth is “non-restorable,” ask your dentist to lay it out for you in plain English, what specifically makes it unstable, and what they consider before making that call.
When you need to seek immediate help
Get to urgent care ASAP if you’re dealing with a fever along with facial swelling, or if you’re having trouble swallowing, breathing, or even just opening your mouth.
What an extraction really means
The tooth extraction procedure involves removing a tooth from its socket in the jawbone due to pain, infection, or other dental issues. It’s a recommendation that can stem from issues like severe decay, infection, trauma, crowding of the surrounding teeth, gum disease, or impacted teeth: it all depends on what your dentist sees when they do an exam.
Before even considering removal, your dentist will often talk about other options like a filling, crown, gum treatment, or root canal therapy. Their goal is conservative care that’s going to last, and they’ll break it all down and walk you through the risks and alternatives.
Pain patterns that get dentists’ attention
Your dental health is important, and all sorts of things could be causing pain in your natural teeth, so don’t try to play doctor and diagnose yourself. That said, there are some pain patterns that are worth taking a closer look at.
Pay attention to severe tooth pain that lingers even after cold or heat has worn off, sharp pain when you’re using pressure to chew, or pain that wakes you up in the middle of the night. Another common pattern is pain that starts to feel better and then just flares up again a few days later.
Infection signs to keep an eye out for, and don’t delay
There are multiple symptoms that, if left untreated, could develop severe further complications to your overall oral health: gum infections can show up as a tender bump, swelling around one tooth, or a bad taste or smell that comes out of nowhere. Some people notice drainage, others mostly just feel a lot of pressure.
Call your dentist immediately if you have swelling or pus visible, even if you’re functioning just fine. Get to urgent care right away if you’ve got a fever along with facial swelling, or if you’re having trouble swallowing or breathing.
Loose teeth and gum disease, don’t wait it out.
If an adult tooth feels loose, don’t try to be patient; it’s often linked to gum disease and bone loss.
Your dentist is going to take a close look at your gum health and get some X-rays to see how much support is still there. Sometimes treatment can help, but other times removal is the best way to go.
Impacted Wisdom teeth and crowding, what’s going on?
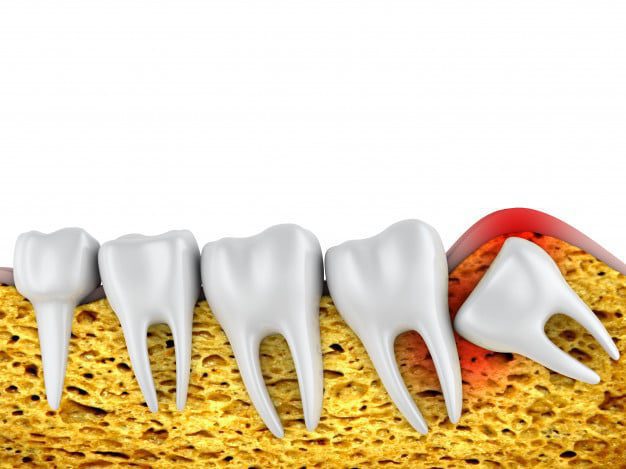
Impacted teeth, especially your wisdom teeth, can cause all sorts of issues: recurring swelling and infection because they’re hard to keep clean. Tooth extractions can be part of the plan when space is needed for additional dental procedures, especially for orthodontic treatment.
If that area keeps flaring up, ask your dentist if imaging might be necessary to check for impaction or related issues.
How dentists determine if you need an extraction
Your symptoms might be a good starting point, but they’re not a definitive answer. Dentists usually confirm extraction needs by combining a good ol’ fashioned exam with some imaging.
That visit might involve an exam, a look at your gums and how mobile they are, and some dental X-rays. It could also include tapping and cold tests to see how sensitive you are and how well you can handle pressure.
Sometimes, a 3D imaging scan (CBCT, cone-beam CT) helps map out the roots, infection, or proximity to nerves. If anything’s still unclear, ask to see the X-rays on the screen and have the dentist point out the exact problem.
What to expect during a tooth extraction
Most extractions fall into one of two categories, and timing and recovery are different depending on which one you get.
- Simple extraction: the affected tooth is visible and can be removed with standard tools
- Surgical extractions: these are required for teeth that are broken, impacted by overcrowded teeth, or deeply rooted, and they might involve a cut, sectioning, and some stitches
After the tooth is successfully removed, the dentist will provide post-extraction instructions and may place gauze over the extraction site to help control bleeding and promote clot formation.
You’ll usually be numb with local anesthesia. A little pressure is normal, but severe pain shouldn’t be, so don’t be afraid to speak up if you’re feeling anything sharp.
Healing and aftercare: what’s normal and what needs a call
Right after an extraction, your body will form a blood clot in the socket & that clot has to be protected for healing to happen properly.
Normal healing will sometimes include a little oozing, some swelling, and soreness that slowly starts to feel better. If any of those symptoms seem off, call your dentist straight away:
- The bleeding just won’t stop after you’ve applied some steady pressure for a bit\
- The pain isn’t getting any better after the second or third day, it’s actually getting worse\
- You get a fever, swelling that gets worse, or a bad taste that returns even after it seemed to have gone away\
- You are having trouble opening your mouth, swallowing, or breathing.
Smoke or use a straw & your dentist will want to make sure you get extra guidance because your risk of getting a dry socket is higher.
Dental Implants, Cosmetic Dentistry… what’s next after the extraction process?
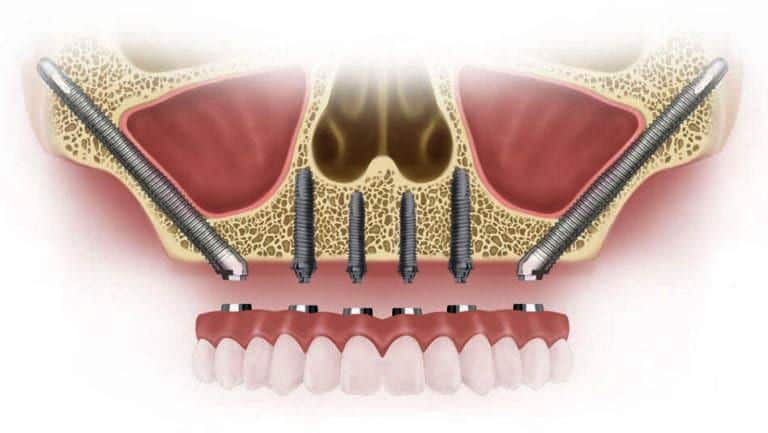
Not every extraction needs a replacement right away, and the timing of replacement is different for everyone.
Whether you need an implant, bridge, or something else to replace your tooth, that’s gonna depend on where the tooth was in your mouth, how your bite is, your gum health, and your overall plan.
If you are planning on delaying replacement, talk to your dentist about your time frame and what you can expect.
Planning dental care in Los Algodones
Los Algodones is a popular spot for dental tourists because it is just down the road from the U.S. border and is set up to handle dental visitors.
Planning ahead is a lot easier when you get some clear guidance before you arrive.
At Dental Solutions Algodones (DSA), we offer a Free Virtual Diagnostic where you send over some recent X-rays and photos, and a timeline of your symptoms, and we will give you some preliminary guidance and a written estimate. The final decisions will be made in person, but you can arrive with a good idea of what to expect.
To be sure everything goes smoothly and the bills are paid, be sure to get everything in writing.
- You’ll get a written estimate that separates the cost for your diagnosis, the type of extraction you need, and what your aftercare is going to be like
- We’ll make sure you have a clear agreement on treatment, but timing and transportation are on you, especially if you need a surgical extraction.
- We’ll provide you with a bilingual consent form and written aftercare instructions.
FAQ: Signs you need a tooth extraction
How can I know if a tooth is beyond repair?
You can tell a tooth is beyond repair when there is not enough tooth structure left to put in a stable restoration or when cracks have gone deep below the gumline. A trip to the dentist and some imaging will give you the definitive answer.
Is a tooth abscess always something I need to rush to the emergency room for?
Not always, but it should be treated pretty quickly. Trouble swallowing or breathing, a fever, and facial swelling are all big red flags.
What is the difference between a simple and surgical tooth extraction?
A simple extraction is one where the tooth is accessible and can be pulled out in a normal procedure. Surgical is when access is difficult, the tooth is chipped or impacted, and they may need to make an incision to get it out.
How long does it take to heal, and can I travel the same day?
A lot of people start to feel better in just a few days, but full socket healing takes much longer. You can usually travel the same day after a simple extraction, but if you have surgical or need sedation, you need to have some extra time to recover.
